Saving Post-Acute Care For Future Generations
By Brian Wallace
January 10, 2024 • Fact checked by Dumb Little Man

Nursing homes are struggling to make ends meet, but why?
Demand for post-acute care grows every year and that trend is likely to continue long into the future. Unfortunately, most people are running out of money before the end of their lives, leaving them reliant on Medicaid for their care. Medicaid reimbursement rates, on the other hand, fall short of the actual cost of care in many facilities.
As the population continues to age, how can we as a society continue to care for our aging loved ones?
Our Population Is Aging

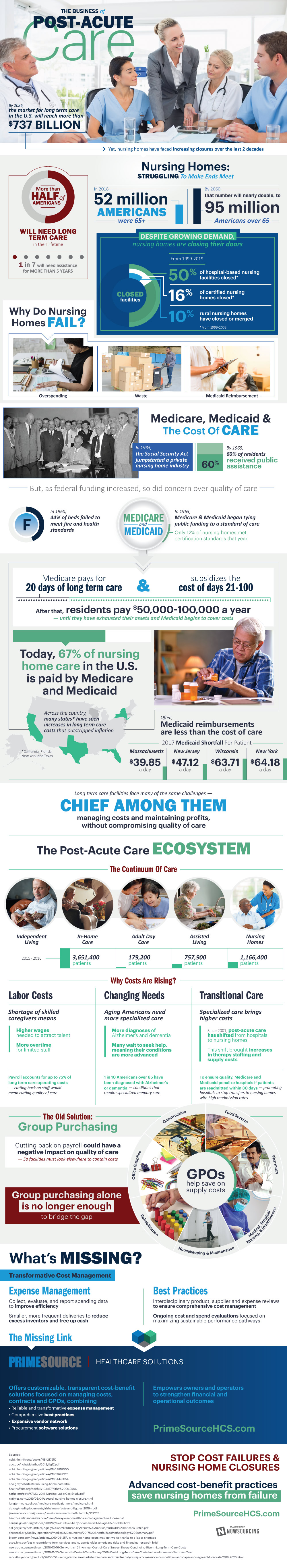
In 2018, more than 52 million Americans were over the age of 65 and by 2060, that number is expected to double. More than half of Americans will need long-term care at some point in their lives for some period of time. One in seven will need it for five years or more.
Despite this demand, facilities that provide these services are closing. Over the last 20 years, half of hospital-based nursing facilities closed, as did 16% of certified nursing homes. One in ten rural nursing homes closed or merged.
Prior to 1935, people who needed care toward the end of their lives were forced to rely on family members or the kindness of the community. This led to a crisis for seniors.
Before the Social Security Act, one in two seniors was forced to move to a “poor house” or panhandle to make ends meet. Any investments they did have didn’t survive the stock market crash. Because the banking industry was largely unregulated, keeping it in a savings account was risky. Those who didn’t have literal money stuffed into a mattress were out of luck.
Social Security aimed to prevent seniors from suffering an undignified end or burdening their communities and families. It provided them an automatic savings plan for their working years, as well as safety net healthcare programs. By 1965, 60% of Americans received public assistance for their nursing home care.
As the age-care industry continued to grow, the need for regulations became clear. In 1960, 44% of nursing home beds failed to meet standards. By 1965, only 12% of nursing homes met certification requirements.
That year, Medicaid and Medicare began tying payments to quality of care. It has helped reduce problems but not eliminate them. It has also created the effect of facilities being unable to recover from mistakes because of the combination of more penalties and lower reimbursement rates.
Today, 67% of nursing home care receives payments from Medicare and Medicaid. The reimbursement rates don’t cover the cost of providing the care the residents need, which is often intensive.
This shortfall varies widely between different markets. In Massachusetts, the shortfall is nearly $40 a day. In New Jersey, it averages just over $47 a day. Meanwhile, in Wisconsin, it’s nearly $64 a day while in New York, it’s nearly $65 a day.
These shortfalls don’t just affect nursing homes – they also affect the post-acute care industry, including adult daycares, in-home care, assisted living, independent living, and more.
See Also: Senior Care- What You Need To Know About Assisted Living
How Can We Save The Post-Acute Care Industry?

Cutting costs in a post-acute care environment is difficult. Labor is expensive because training is necessary. Plus, the people who provide care need to have a certain level of skill in order to provide a quality of care that meets standards. The cost of facilities and labor have to remain high because of standards.
In the past, the only place to trim spending was in purchasing through group purchasing organizations.
Today, there are more ways than just group purchasing to curb post-acute care costs and, in effect, extend a better quality of care to patients without the threat of a facility closure. Data management may be useful in analyzing how to improve efficiency. Frequent and smaller deliveries may free up cash. Adhering to best practices can help already struggling post-acute care businesses make ends meet.
Learn more about the business of post-acute care and how it can be streamlined so it can last for future generations that will need it from the infographic below.
Source: PrimeSource
Brian Wallace
Brian Wallace is the Founder and President of NowSourcing, an industry leading infographic design agency based in Louisville, KY and Cincinnati, OH which works with companies that range from startups to Fortune 500s. Brian also runs #LinkedInLocal events nationwide, and hosts the Next Action Podcast. Brian has been named a Google Small Business Advisor for 2016-present and joined the SXSW Advisory Board in 2019.